Fetal Ductus Venosus
The findings of recent studies suggest that examination of the ductus venosus waveform at 11-13+6 weeks could have major beneficial implications in screening for Trisomy 21 by maternal age and fetal nuchal translucency (NT). However it is imperative that, as for the NT scan, sonographers undertaking risk assessment by examination of the fetal ductus venosus waveform must receive appropriate training and certification of their competence in performing the ductus venosus scan.
Protocol for the assessment of the ductus venosus
- The gestational period must be 11 to 13+6 weeks.
- The examination should be undertaken during fetal quiescence.
- The magnification of the image should be such that the fetal thorax and abdomen occupy the whole image.
- A right ventral mid-sagittal view of the fetal trunk should be obtained and color flow mapping should be undertaken to demonstrate the umbilical vein, ductus venosus and fetal heart.
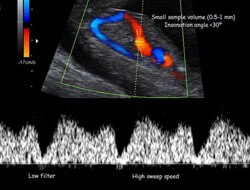
- The pulsed Doppler sample volume should be small (0.5-1 mm) to avoid contamination from the adjacent veins, and it should be placed in the yellowish aliasing area which is the portion immediately above the umbilical sinus.
- The insonation angle should be less than 30 degrees. The angle correction tool must be used to show that the angle of flow is Less than 30 degrees.
- The filter should be set at a low frequency (50-70 Hz) so that the a-wave is not obscured.
- The sweep speed should be high (2-3 cm/s) so that the waveforms are spread allowing better assessment of the a-wave.
When these criteria are satisfied, it is possible to assess the a-wave and determine qualitatively whether the flow is positive, absent or reversed
Clinical application of ductus venosus findings The incidence of reversed ductus venosus a-wave is related to NT and CRL as well as aneuploidy, being more common with increased NT and smaller CRL measurements. Therefore it is not possible to give simple numbers by which the presence of normal flow will reduce the risk for Trisomy 21 and the presence of reversed a-wave will increase the risk. It is essential that those adjusting the risk for Trisomy 21 using the finding of tricuspid flow do so with recognized risk calculation software that take into account all the appropriate parameters. The Fetal Medicine Foundation will release such risk calculation software, but will only make it available to sonographers who have been appropriately trained and accredited in the assessment of the fetal ductus venosus wave-form.
The software firstly calculates a risk based on maternal age, fetal nuchal translucency and maternal serum free ß-hCG and PAPP-A. If the risk is more than 1 in 50 and ductus venosus flow is normal the risk does not change. If the risk is 1 in 50 to 1 in 1,000 and the ductus venosus flow is normal the risk is usually reduced. If there is reversed a-wave the risk is always increased. In addition, there is an increased risk for cardiac defects and therefore such patients should have a follow up specialist fetal cardiac scan.